High Tech Benefits Minimally Invasive Surgery. What Does the Future Hold?
Minimally invasive device technology and surgery are becoming accepted practices in modern healthcare. But where is it going?
July 30, 2021
Philip Remedios
Since the turn of the century, advancements in capability using Minimally invasive surgical (MIS) techniques have been nothing short of miraculous. For this article, I have chosen to include interventional procedures (involving trans-vascular anatomical access) within the minimally invasive surgical toolkit, including endoscopy, laparoscopy, arthroscopy, and robot-assisted surgeries. However, the primary physician is different in each case. Skillsets in modern surgery coupled with impressive new technology and devices have enabled what was once highly invasive procedures to be conducted using minimal incisions, instrument/scope access (trocar or “keyhole”) ports, and sometimes just small diameter catheter vascular access.
MIS's advantages to healthcare include reduced patient trauma and discomfort, less opportunity for infection, faster procedural and recovery times, which usually means reduced healthcare costs. However, the need to perform highly skilled actions using specialized tools with limited visibility and ranges of motion has introduced higher levels of expertise for the surgical team, from endoscopic surgeons, robotic procedure specialists to interventional radiologists. Support equipment includes endoscopic cameras, visualization scanners, contrast injectors, non-magnetic monitors, specialized instruments and catheters, and expensive robotic systems. Despite the setup overhead for MIS, there is no disputing the value these advances in surgical procedures bring to the industry. Today’s MIS infrastructure is pronounced and widespread in every healthcare sector.
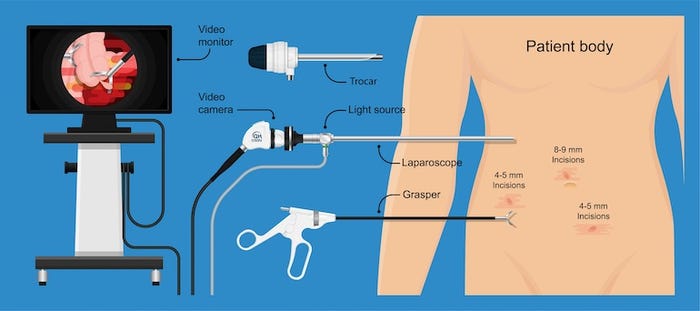
MIS Device Design Trends
The devices required to support MIS techniques continue to proliferate at impressive levels. Instruments have become highly specialized in doing a specific task swiftly without requiring too much technique from the user. The number of individual designs available today to surgeons is quite daunting. It is not uncommon for a power user (Key Opinion Leader or KOL) to develop their version of a device based on their specific technique, becoming a unique offering by a partnering manufacturer. Miniaturized sensors and electronics can be integrated into the tips of these handheld instruments or within tiny catheters to monitor pressure, blood flow, and electrical fields, providing clinicians with vital anatomical feedback while working virtually blind. Combined with these sensors, some devices even offer synthesized input to the user, which may be in the form of haptic vibration and mechanical resistance, visual and audible instructions.
Robot-assisted surgery has become a fast-moving technology that enhances the accuracy of complex surgeries while reducing patient trauma and recovery time because robots do not need direct visualization of the surgical site. Robots may be as simplistic as a smart guidance fixture for probes and cannula insertions or as complex as a floor-standing multi-tool device that can operate remotely on patients from across the globe, controlled by skilled surgeons via advanced telemetry. Military leadership has aggressively pursued technology to enable this interoperability to vastly enhance the survivability of wounded service members in the field. Robots are now commonplace for orthopedic procedures such as knee and hip replacements and prostate surgery, where the level of precision provided by the robotic guidance far exceeds even the most skilled surgeon. Combined with 3D-imaging and real-time interpolated anatomical modeling, robot-assisted surgical efficacy drives the proliferation of targeted robotic platforms into most surgical and oncologic procedures.
MIS has its challenges - the cost of capital equipment such as imaging systems and robots can be prohibitive and specialized training of personnel requires a team of dedicated clinicians and facilities. Cath labs have replaced many operating rooms as the value and effectiveness of interventional procedures have proven themselves in treating coronary disease. It is simply extraordinary to understand that today we can have our aortic valves replaced via femoral artery-accessed catheter delivery, requiring no thoracic surgical access. Tiny pumps integrated into the ends of catheters can help us pump blood from the ventricle to the atrium until our hearts heal from a procedure and usually operate.
Visualization Technology
Visualization requirements associated with MIS rely on sophisticated technology to enable the clinician to see “through” anatomy. Without these advances, most MIS procedures would be impossible to perform with the required levels of accuracy and reliability. Camera CMOS sensors have become so small and affordable (thanks to the consumer products industry) that articulating scopes can now visualize anatomy in a high-resolution video that was simply impossible just a decade ago. Features such as tissue texture and relative coloration can be assessed in real-time due to HD-enhancing and color-correcting software, a performance upgrade vital to tasks such as abnormal tissue identification. Along with the physical hardware is software that can interpolate scanned anatomy to provide 3-dimensional images, perhaps overlaying pre-scanned patient anatomy to help guide the user around tortuous pathways during device implantation.
Magnetic Resonance Imaging (MRI), Computed Tomography (CT), X-Ray, Ultrasound, Fluoroscopy, etc., are all mature technologies but recent advances in digital image enhancement coupled with computer processing power significantly enhance resolution for MIS applications. MRI imaging has a unique problem: any equipment in the MRI suite must be non-ferrous to resist the massive magnetic fields created by the scanner. Patients that require 24/7 hook-up to critical-care monitors and life support devices such as ventilators, pumps, and monitors rely on these special MRI-compatible devices. CT imaging involves the introduction of contrast solution into the patient’s vasculature to provide an appropriate image, with the ability to customize the consistency of the contrast solution to “match” the particular patient’s anatomy to optimize image clarity. Modern injectors provide a plethora of settings, including pre-set and custom ratios of the contrast-to-saline fluid mix, pressure, and ramp profiles. Ultrasound (U/S) imaging most recently has perhaps offered the most incredible opportunity to caregivers as it is a compact (briefcase-sized), simple, safe, inexpensive technology. As a result, U/S is increasingly being paired up with a broad base of diagnostic and simple therapeutic procedures in outpatient and doctors’ office settings.
An example of this is the imaging of air-infused saline for fallopian tube patency. The saline-based contrast medium and imaging system are far cheaper and inherently safer than other traditional imaging methods. It is easy to extrapolate the transition of U/S imaging into home-health telemedicine (distance-care) in the future, including patient-operated fetal monitoring.
User-Centered Design in MIS Devices
Beyond the availability of cutting-edge instruments and devices, MIS specialists have to develop specific skill sets. While open-heart surgery certainly requires immense skill in its own right, imagine performing a trans-catheter aortic valve replacement entirely from a groin-area access site! External grips at the end of long cannulae or worse, hub-located control interfaces at the proximal end of a two-meter-long, spaghetti-like catheter must provide the ability to push, pull, turn and activate features deep inside the body. Whether we are reviewing laparoscopic or interventional techniques, consider the lack of direct interface, low-to-zero tactile feedback coupled with compromised visualization.
It is easy to understand how important these MIS devices are to minimize error modalities due to poor ergonomics, repetitive stress, and non-intuitive control design. When the clinician’s “eyes” are the camera monitor, they should not have to refocus on the device in hand because they cannot find the actuator or adjustment feature! To assist with these challenges, some devices can be coupled to controllers that help provide feedback such as temperature, pressure and flow sensing, and high precision deployment of miniature tools integrated within the distal tip of the embedded device to perform the procedure. These controllers can help the operator “feel” their way around the anatomy, providing continuous monitoring of critical parameters.
Device manufacturers are always searching for ways to “de-skill” the MIS process so that the average operator can likely succeed without requiring rigorous training. To this end, some designers have tried synthesizing feedback into their devices. This may involve adding electromechanically-generated haptic (vibration, pulsing, resistance), audible and visual feedback to denote various functional states during the procedure. Unfortunately, most of these devices are also single-use in nature, so unit costs must also be contained, which adds to the challenges to optimizing ergonomics. One strategy is to build these feedback features into a durable (reusable) part of the device so that the cost can be amortized over many cases. Miniaturization (nano) technology has also advanced to the point where the cost of “medical-grade” embedded sensors is becoming affordable while accurate enough to be useful.
What’s the future of MIS technology?
Despite the incredible growth in MIS advancements over the last two decades, these techniques are still in their adolescence, and there is much room for growth. As component performance increases and cost decreases, we can expect to see the convergence of many technologies, particularly from the electronic and digital industries, that will enable device manufacturers to deliver smaller, more accurate, and less expensive devices that are easier to operate a growing range of procedures. Much in the same way that transcatheter aortic valve replacement has truly been a disruptive innovation, miniaturized robotics, nano-actuators, electronics, and higher-definition optics can provide even greater remote functionality at the end of a laparoscopic cannula or vascular catheter. There has been speculation that tiny, preprogrammed “robots” may one day be injectable into the bloodstream or pulmonary airway where they autonomously do the job of surgeons with perhaps no trauma to the patient. Biologically engineered viruses (similar to recent mRNA COVID vaccines) may also be capable of functioning at the cellular level to obliterate cancer and other abnormalities throughout the human body. Although these scenarios may sound like they have been pilfered from the pages of scientific journals, one fact is clear- medical technology in the minimally-invasive space is accelerating faster than ever in an effort to do more with less, which can only benefit across the entire healthcare continuum in the long run.
Philip Remedios is the Principal and Director of Design & Development at BlackHägen Design.
You May Also Like

.jpg?width=300&auto=webp&quality=80&disable=upscale)